Updated 6/15/21

There are several different periodic fever syndromes (PFS). Each have different treatment options. Graphic by The Flying Lifeguards
Periodic fever syndrome does not refer to a single disease, nor is it a specific diagnosis, but rather a general term, a classification of a group of diseases.
The term “periodic fever syndrome” refers to several different autoinflammatory diseases that have similar symptoms–the primary symptom being a recurrent fever for which no infectious cause can be found. The patient just keeps getting fevers, often accompanied other inflammatory symptoms.
These are primarily genetic conditions and are not contagious. Autoinflammatory diseases are caused by a malfunction in the innate immune system that leads to an over active immune system. This over activation causes severe systemic inflammation throughout the body.
The periodic fever syndromes include, but are not limited to:
- The Cryopryin-Associated Periodic syndromes (CAPS): Familial Cold Autoinflammatory Syndrome (FCAS), Muckle-Wells Syndrome (MWS), and Neonatal-Onset Multisystem Inflammatory Disease (NOMID or CINCA)
- Familial Mediterranean Fever (FMF)
- Tumour Necrosis Factor (TNF)-Associated Periodic Syndrome (TRAPS)
- Mevalonate Kinase Deficiencies: Hyper-IgD with Periodic Fever Syndrome (HIDS), and Mevoalonate Aciduria (MA)
- Periodic Fever, Aphthous Stomatitis, Pharyngitis, & Cervical Adenitis (PFAPA syndrome)
- Familial Behcet’s-like autoinflammatory syndrome
- And several others. Click here to see a full list.
Common Periodic Fever Syndrome Symptoms
Many autoinflammatory diseases (these are NOT autoimmune – click here for more) tend to have frequent recurring fevers as the most obvious symptom. The fevers are often cyclic in nature, coming and going in some cases erratically and in some cases more predictably. However much more is going on than just a fever inside the body. These diseases cause the rapid onset of intense episodes of systemic inflammation that can affect multiple organs and tissues. Which body systems are most affected depends on the specific syndrome.
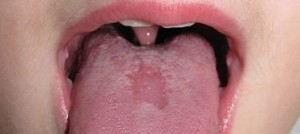
This mouth ulcer in a PFAPA patient is healing. Mouth ulcers are common in several autoinflammatory syndromes, including DIRA, HIDS, TRAPS, and FMF.
These are some of the most common symptoms that may be noted during disease flares in various periodic fever syndromes:
- Fever (recurrent, and accompanied by some of the following symptoms)*
- Rash
- Headache
- Vomiting
- Diarrhea
- Constipation
- Conjunctivitis
- Mouth ulcers
- Swollen lymph nodes
- Abdominal pain
- Joint pains, or arthritis
- Fatigue
- Abnormal blood test results during flares of symptoms, including: high white blood count (WBC) and high inflammatory markers CRP and ESR
- Serositis (pericarditis, pleurisy)
*Some will have on-going symptoms listed above without a fever.
Age of Onset
Most patients start presenting with symptoms in childhood before the age of 5. However, some patients may not develop their first symptoms until they are older (school age or adolescence) or even as adults.
Prognosis
Like the symptoms, the prognosis for someone living with a periodic fever syndrome often depends on which syndrome he or she has. For some, like those with PFAPA, the prognosis is considered good, as PFAPA is typically outgrown. For most others, these are lifelong conditions that must be managed with medication to prevent serious complications from the disease. In some cases, the disease may go into remission for months to years at a time.
Getting a Specific Diagnosis for a Periodic Fever Syndrome
Many of the periodic fever syndromes are also referred to as “hereditary periodic fever syndromes,” because they are caused by genetic mutations. Some mutations are dominantly inherited (meaning you only need one mutation to cause disease), and others are recessively inherited (where you need to inherit two mutations to develop the disease.)
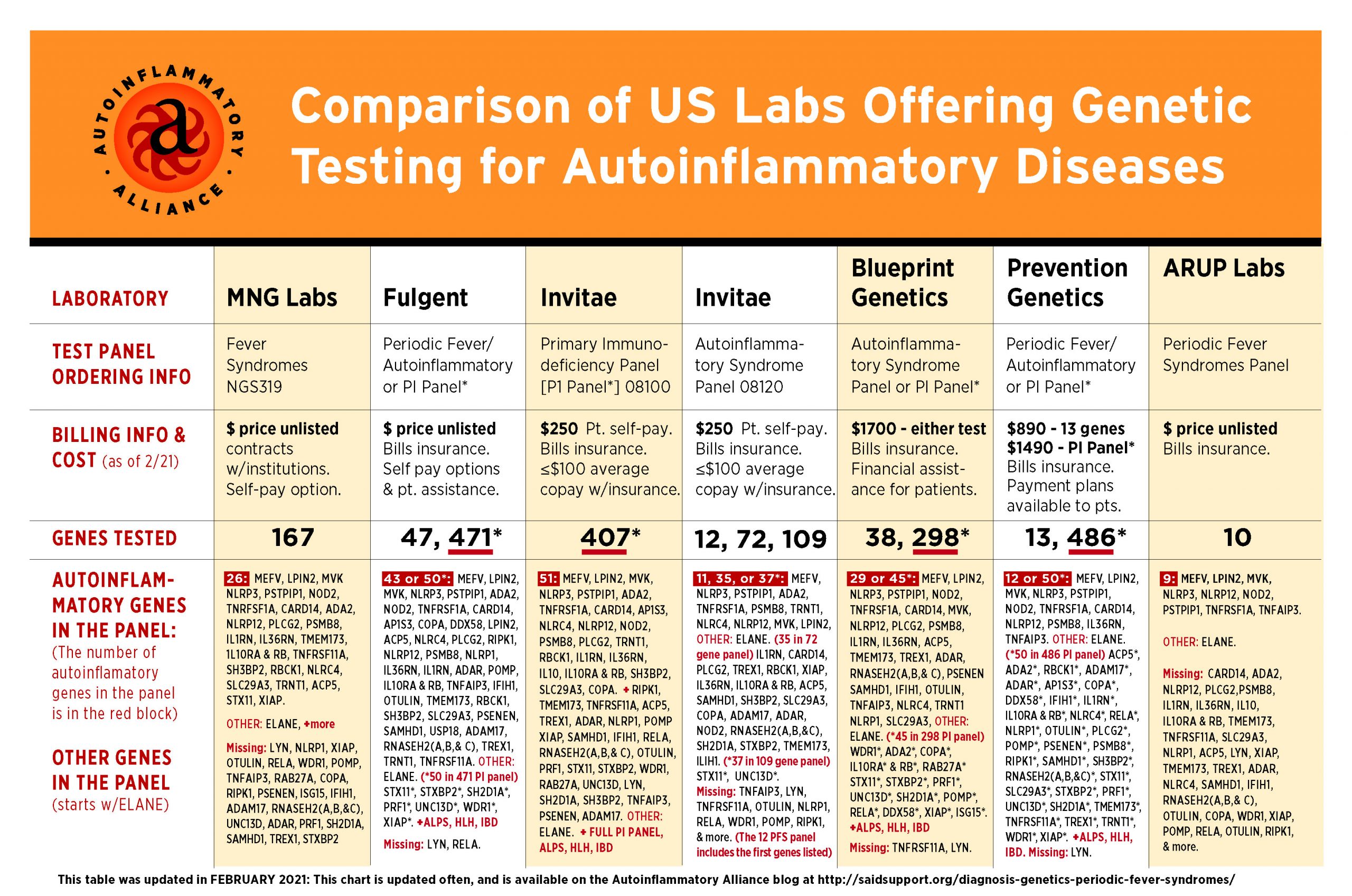
As of 2021, Invitae has one of the most comprehensive and budget friendly genetic panels for autoinflammatory diseases. Click here to see that panel.
Once a patient is suspected of having a periodic fever syndrome, it is necessary for the doctors to first do a clinical evaluation to try to determine which syndrome(s) could be a possibility. This includes an evaluation of the patient’s most common symptoms, blood tests (during flares of symptoms, and during times with no obvious symptoms), and genetic testing for these diseases. If the patient has a rash, a skin biopsy by a dermatologist should be done as well.
For some conditions, a genetic test is not yet available, such as for PFAPA. However, it is ideal to rule out the known hereditary periodic fever syndromes, such as FMF, MWS, HA20, and HIDS, when diagnosing PFAPA, since these diseases have similar symptoms. PFAPA is too often diagnosed without a full attempt to rule out the other autoinflammatory diseases, and therefore too often misdiagnosed. A misdiagnosis of PFAPA, if the patient has another periodic fever syndrome, can delay starting medications that are most effective and can prevent risks and complications of their disease. Other autoinflammatory diseases can share the same symptoms as PFAPA, but need different treatments to manage the disease and reduce the risk of serious complications.
Classic PFAPA patients are considered to be symptom-free without signs of chronic inflammation in between attacks of the fever. They also do not have elevated inflammatory labs when they are not having the fever flares. However, this can also occur in some patients with other autoinflammatory conditions such as HIDS.
If a patient has signs of enduring symptoms between times of the fever, or elevated inflammatory markers on lab tests when they are not flaring, or additional symptoms beyond the list above, other autoinflammatory diseases beyond PFAPA must be considered. Concerning symptoms of chronic inflammation include: an enlarged liver and/or spleen, progressive hearing loss, inflammation in the eyes, growth delays, neuro-cognitive deficits, persistent rashes, vasculitis, or an other unusual, chronic signs of inflammation.
Conditions Similar to Periodic Fever Syndromes
When patients have recurring fevers and other inflammatory symptoms, doctors will consider several differential diagnosis for conditions that can have similar symptoms. These include immune deficiencies, autoimmune diseases, mast cell activation syndrome (MCAS) just to name a few. The larger and cost-effective immune dysregulation genetic panels include many of these differential diagnosis along with autoinflammatory genes.
Do you have recurring fevers and need help? Follow the links below for more help.
The Autoinflammatory Alliance is a nonprofit organization dedicated to helping those with autoinflammatory diseases.
Donate now to help with awareness, education, and research for these rare diseases.
References







My son had periodic fever syndrome. He would get 105 degree fevers every 13 days. This continued for almost 2 years until I read on the Internet about how tonsillectomies usually cure the problem. Five doctors couldn’t come up with any answers, so I took him to an ENT. He had his tonsils out and hasn’t had a fever since. It’s been 8 months. I know this doesn’t work for all types of recurring fevers, but it did for my son.
HI Sue,
Thank you for sharing your story. Tonsillectomy is known to help some with PFAPA. Unfortunately it isn’t known to help with any of the other periodic fever syndromes which is why having a good diagnosis first helps.
We have more information on PFAPA here – http://saidsupport.org/list-of-periodic-fever-aphthous-stomatitis-pharyngitis-cervical-adenitis-syndrome-pfapa-research-and-information/
And how fever syndromes are diagnosed here – http://saidsupport.org/patient-resources/finding-a-diagnosis/
Jennifer
My child has periodic fever syndrome has 40+ temperatures every 20/28 days persistent leg,arm stomach pains which can be severe to the point she wants her limbs cut off so can be really painful,vomiting ,fitting ,lethargic ,diareah constantly .Have been referred to a number of pediatric consultants but still no diagnosis as such ,we are due to have ultra sound scan for kidneys as uti infections have been noted at times but not always the cause usually doctors put it down to a virul infection which usually means they don’t no what’s causing her illness she is only 3yrs old so this is ongoing her bloods show her immunoglobulin 1gA is borderline low has recently had bloods whilst poorly for inflammatory markers still awaiting results
Hello Lynne,
I’m sorry to hear your child is suffering like this. I’d like to give you some resources to help. It looks like you are in the UK? The Periodic Fever Service at the Royal Free are experts in these diseases. It would be good to get a referral there. This is more info on them – http://www.amyloidosis.org.uk/fever-syndromes/the-periodic-fever-service-at-the-nac/
This is the autoinflammatory database that you can go over and discuss anything that stands out to you with your doctors – http://www.autoinflammatory-search.org/diseases
Also, please feel free to join our Facebook group where you can find others who have similar symptoms – https://www.facebook.com/groups/nomidalliance/
I hope this helps and you can get answers and treatment soon.
Jennifer
I am having fever periodically every 20-30 days and when i work hard physically then fever occur,please help me and suggest good doctors name in INDIA,if possible then let me know also about BIHAR
Hello Amar,
Please email Karen Durrant at Karen at autoinflammatory.org. She may know of doctors for you to see.
Jennifer
I am 59 and have been having recurring fevers that just began within the last year. I get these fevers (my latest was 102F) for one day and after a good night’s sleep, the fever is gone. These come on all of the sudden and I have fatigue. I have tried to pinpoint when these occur and what brings them on and the only thing I can think of is after I exert myself a lot. It will be 2-3 weeks before I have another fever. I did go to my PCP and took him a list of my symptoms when I feel like this. He ordered a CBC and my white blood count came back 20.1. He said he wasn’t concerned and said he thought I was fighting a bug. Fighting a bug for 8 or 9 months? What are your suggestions? Thanks.
Hi Jayne,
It sounds like more testing is needed to see what is going on. In particular CRP and ESR need to be testing both when in a fever and when not in a fever along with the WBC. This goes over initial bloodwork that is needed – http://saidsupport.org/child-keeps-getting-fevers/ As you can see from that article, WBC is often high in fever syndromes because the body things it is fighting a virus, but there is often not a virus.
Some specialists to see would be an infectious disease doctor to look for some kind of chronic infection and a rheumatologist to evaluate for an autoimmune or autoinflammatory disease.
Also we can help more if you join our Facebook group – https://www.facebook.com/groups/nomidalliance/
Hope this helps!
Jennifer
Hi I’m 28 and I’ve been feeling so bad that I’m ready to give up lately. It never ends. I get fevers at least 5 times a week. Headaches, diarrhea, I’m so tired and when it’s hot outside also it’s almost unbearable. I have thought that it was all in my head until seeing this. I live in West Virginia and have a state medical card as I also have DDD, two herniated discs, a pinched nerve, and am constantly battling pain and anxiety. Please help me if you know any doctors in my area that would take a medical card.
Hello Kandi,
I am very sorry to hear you are suffering like this. Please email Karen Durrant at Karen@autoinflammatory.org as she may have doctor recommendations for you. Also please join our Facebook group. There you can find others with similar symptoms and more doctor recommendations.
https://www.facebook.com/groups/nomidalliance/
I hope you can get help for this soon.
Jennifer
My son (age 2) has been having fevers once a month it seems, and with no other symptoms. And I have other children that are not sick. The highest it’s ever been was 102.8 and I use infant Tylenol to bring it down. I’ve made the earliest appointment for him july13 with his doctor. I keep worrying that it’s something like lymes disease.. we love I’m a area where finding ticks is normal. but he’s never had a large sore like a bullseye or any other rashes. He loses his appetite while the fever is high and drinks pleanty. He doesn’t seem to have aches in his body, but he does seem more tuckered out while the fever is preasent.
Hello Vera,
I’m sorry to hear your son is suffering with monthly fevers. The periodic fever syndromes for the most are genetic are not infections, but it is good to see an Infectious Disease specialist to help figure this out as they can best check for an infectious cause. This article goes over blood tests that are needed and other things to talk to the doctor about – http://saidsupport.org/child-keeps-getting-fevers/
Also you are welcome to join our FB group – https://www.facebook.com/groups/nomidalliance/
I hope this helps and you can get some answers soon.
Jennifer
Hello.
My daughter is 19 months old and this all started when she was around 6 months.
It all begin with your typical dr visited that was passed off as a viral infection and the more than you’d like to hear “kids get sick”
But after numerous hospital visits of recurring fevers that always started every 3 weeks and would last five to seven days. Doctor started seeing a pattern as well as my husband and I did. So many more symptoms started showing up over the last year. My daughter has extreme swelling in her knees, jawline,ankles, feet, wrist, hands and around her eyes.
Fleshy rashes that occurs during her 106 fever.
Seizure-like activity that’s led to an EEG and possibly MRI.
As well as light sensitivity and hitting her head over and over again as if she had headaches.
Busted blood vessels in her face and ears
test after test and finally after seeing an immunologist we were referred to a Rheumatology specialist.
After going back and forth thinking it was lupus The Specialist narrowed it down to autoinflammatory disease or / and periodic fever syndrome.
We were told they had to send out a pre-authorization for a genetic mutation testing because the test cost $5,000.her inflammatory markers are usually on the rise as well as a few other test. We were asked to write a detailed diary which we already have been for a while in between testing. My daughter has suffered so long. She’s actually in my arms right now going through a flare up.they worse each time!
I’m ready to get answers. I don’t care about the insurance I will figure out a way to pay for the testing. My daughter needs treatment. But from what I have read and heard there is not a lot of treatment out there other than a life time of steroids which have their own effect. Any advice out there? My heart hurts for my daughter.
Her Flair are so painful she cannot get up.
She’s only 19 months old we were referred to a therapist so she can learn how to cope with this illness. My head is in a world wind watching my baby grow through this
my 16 yo daughter has frequent fever monthly.pain all over her body during night time.any recommendation pls.thank you
Hello,
I’m sorry to hear your daughter is suffering like this. Your daughter would need some bloodwork and to see some specialists to help figure this out. This post goes over what to do and what to talk to her doctor about – http://saidsupport.org/child-keeps-getting-fevers/
Also you are welcome join our Facebook group. There you can find others with similar symptoms and more help with finding doctors who know autoinflammatory diseases. https://www.facebook.com/groups/nomidalliance/
I hope this helps.
Jennifer
Hello Amanda,
It sounds like you are getting in the right direction for getting answers to what is going on. The genetic testing can be very helpful for a diagnosis, however none of the genetic fever panels cost $5,000. The MNG panel which tests for the most syndromes at one time is the least expensive at $1320. Please share this post with your doctors – it covers the currently available panels. http://saidsupport.org/patient-resources/finding-a-diagnosis/
As for treatment, there is absolutely treatment for most of these diseases. I would ask your doctor about what options there are besides prednisone. Please join our Facebook group Autoinflammatory Diseases-Rare But Not Alone and we can give you more help there. https://www.facebook.com/groups/nomidalliance/
I hope this helps and I look forward to “meeting” you in our FB group.
Jennifer
Im looking into trying to find out what’s wrong with my nephew. He is 3 and for about a year now he is continuously having fevers. He sometimes vomits, diarrhea, and rash around the mouth. This is my sister’s first child and I can’t give her much advice because my 3 children never had fever’s that reoccurred as often as his. It seems to come every 14-18 days. I told her this seems strange. The doctor’s keep saying it could just be a virus. I’m worried that it could be something more serious. What advice can I give her?
Hello,
You can share this post with your sister – it goes over what to do and discuss with the doctor when someone is getting unexplained recurring fevers. http://saidsupport.org/child-keeps-getting-fevers/
Also you and your sister are welcome to join our Facebook group – Autoinflammatory Diseases – Rare But Not Alone. https://www.facebook.com/groups/nomidalliance/
I hope this helps!
Jennifer
Hi can you suggest what specialist to see with periodic fever syndrome to find out what type it is? My daughter’s pediatrician believes she may have it. She suggested going to an ent to get her tonsils out but upon further research it seems like more tests should be done to make sure it’s the type will respond to a tonsillectomy.
Hello Tabetha,
These diseases fall mostly under the rheumatology specialty, so you would want to ask for a rheumatologist referral. If you join our Facebook group you can get recommendations from others in your area. https://www.facebook.com/groups/nomidalliance/
Jennifer
I’m currently 21. (male) For the last 10 years or so I’ve had periodic fevers. When it started back in 7th grade it would be once every few months, later on in high school it picked up to every couple months and now it’s once a month at least. They almost always last for one day only and after sleeping, (or if it’s two days, same thing but the second night) I’m fine. I’ll sometimes have a soar throat and sinus pressure, but not always. They’re not contagious and not a flu/common cold. I’ve talked to my doctor and Mom, (an RN) and neither of them could figure out what it was. This is getting worse and I’m scared it could be something really wrong with me. I used to not worry because they were so infrequent, but now it’s as often as it is I’m worried.
Hello Alex,
I’m sorry you haven’t been able to get help for your symptoms. A rheumatologist is usually best to evaluate for a fever syndrome.
This post goes over what to talk to your doctor about to start figuring this out – http://saidsupport.org/child-keeps-getting-fevers/
Also please join our Facebook group – Autoinflammatory Diseases – Rare but not Alone. There we can get you more help and you can meet others who have similar symptoms. https://www.facebook.com/groups/nomidalliance
I hope this helps!
Jennifer
My blood pressure is 138/93. I don’t know about the readings it says MR- 86/ mt SPO2 98%. My sugar level was 141. Am having frequent fevers and was troubled due to no dysentery. With medications i am having relief. But the fever is making me uncomfortable.
Hello,
I’m sorry you haven’t been able to get help for the fevers. A rheumatologist is usually best to evaluate for a fever syndrome.
This post goes over what to talk to your doctor about to start figuring this out – http://saidsupport.org/child-keeps-getting-fevers/
Also please join our Facebook group – Autoinflammatory Diseases – Rare but not Alone. There we can get you more help and you can meet others who have similar symptoms. https://www.facebook.com/groups/nomidalliance
I hope this helps!
Jennifer
Hi my son is 18 months he’s had extremely high fevers of 104 to 105.1 on and off for 8 months now, there’s no other symptoms besides they always tell me he has lots of lymph nodes and a red throat wich they have ta Ken more than 10 cultures for strep all negitive. Finally took blood tests all very high for a good 5 months it went down then back up (white blood cell count and platelets) he also had a couple of other things in his blood test that were very weird he has been tested for leukima multiple times but no blasts cells only one they had said in the beginning but no more. He has been getting worse 105 fever febrile siezers and very lethargic we had to call 91 because he wasn’t responding the hospital told us that he needed to go back to the hemotologist to figure this out but we have been to the hemotologist 3 times a oncologist a gi doctor a allergist doctor and his pediatrician his fevers last up to 3 days then he’s totally fine then he’s at it again I just feel so bad 🙁 not sure what to do anymore
Hello Ashley,
I’m sorry you are going through this with your son. A rheumatologist is usually best to evaluate for a fever syndrome.
This post goes over what to talk to your doctor about to start figuring this out – http://saidsupport.org/child-keeps-getting-fevers/
Also please join our Facebook group – Autoinflammatory Diseases – Rare but not Alone. There we can get you more help and you can meet others who have similar symptoms. https://www.facebook.com/groups/nomidalliance
I hope this helps!
Jennifer
i am 56years old male – for the last 5 months am getting fever every 5or 6 days which lasts for a day- was on anti biotic n steriods but now not on any medication except panadol whenever i have fever- fever ranges from 37.3 to 38 -have done more than 10 blood test n cancer test n all test that the doctors reccomended but all are negative! i get pain in my knees n legs whenever i have fever –can anyone help me– have seen all doctors
Hello, J Bajaj,
I’m sorry you are dealing with periodic fevers. An infectious diseases doctor can help rule out an infectious cause. Immunology and rheumatology can look for immune deficiencies and autoinflammatory diseases.
This post goes over what to do and discuss with the doctors when trying to figure out the cause of recurrent fevers – http://saidsupport.org/child-keeps-getting-fevers/
Also you are welcome to join our Facebook group to get more help – https://www.facebook.com/groups/nomidalliance/
Jennifer
hoi my son is 5.5 years old he us having fever last 7 month its go on every Friday and Saturday he us having headache stomach pain vomiting can’t understand what to do very much tensed coluld u help to please .
Hello Isha,
A rheumatologist is usually best to evaluate for a fever syndrome. This post goes over what to talk to your doctor about to start figuring this out – http://saidsupport.org/child-keeps-getting-fevers/
Also please join our Facebook group – Autoinflammatory Diseases – Rare but not Alone. There we can get you more help and you can meet others who have similar symptoms. https://www.facebook.com/groups/nomidalliance I hope this helps!
Jennifer