Updated 04/19/22

In periodic fever syndromes, patients get regular fevers along with other symptoms without an obvious cause. Photo by silroby/Bigstockphoto.com
If you or your child keeps getting fevers, there could be several causes. These can include periodic fever syndromes, recurrent infection, immunodeficiency syndromes, mast cell activation syndrome (MCAS), or autoimmune diseases. The periodic fever syndromes, also known as autoinflammatory diseases will be discussed here.
It’s hard for doctors to distinguish between a periodic fever syndrome and normal viral illnesses in children with recurrent fevers as frequent illnesses are common in young children. Even for adults who less commonly have frequent fevers, doctors will consider infections first.
Doctors do not want to miss something that may be an infection that needs immediate treatment, such as strep throat. Often, it is not until a child or adult shows a pattern of fevers and other symptoms over several months where they have no infections detected that doctors start to consider the need to evaluate the patient for periodic fever syndromes.
This can be very frustrating to patients and their families, but there are few things you can do during this process to help with finding a diagnosis.
What are Periodic Fever Syndromes?
In the autoinflammatory diseases, which includes the periodic fever syndromes, the fevers are often the most obvious symptom. Fevers are accompanied, or are quickly followed by other symptoms throughout the body. These can include rash, joint pain, stomach pain, chest pain, mouth ulcers, headache, red eyes, and extreme fatigue.
In fever syndromes, the flares are often distinct, increasing in severity for days to weeks and then improving without explanation. The additional symptoms will usually also increase and decrease with the fever.
In some syndromes, the symptoms are more chronic and do not have periods of improvement.
Click here to learn more about periodic fever syndrome symptoms.
If you suspect you or your child has a periodic fever syndrome, you will need to start with your primary care doctor to discuss your concerns and symptoms.
Here are the steps to take if you or your child is having recurrent fevers without explanation. All of the information and resources here are intended to be shared with your doctors.

When taking a temperature, always record the temperature and any other symptoms. Photo by art_of_sun/Bigstockphoto.com
1. Keep a Fever and Symptom Log
Log the dates of the fevers and temperature and note the time the temperature was taken. The fever pattern can be very helpful in diagnosing. Some autoinflammatory diseases have continuous nonstop fevers over several days, while others, such as SJIA have fevers the recur in the afternoons or evenings. Also keep a log of any symptoms you notice. Include every symptom that’s possibly related for now. Some symptoms may not be related, but when starting the diagnostic process include everything for evaluation and to see if a pattern emerges.
Note when the fever and symptoms start, and end by hours, or days on the log. This is very helpful for doctors, as various autoinflammatory diseases have different fever patterns and accompanying symptoms.
Click here for a list of different symptom logs many autoinflammatory patients use.
2. Make a List of Important Developmental Milestones, Growth, and Vaccinations
Go through your child’s baby book, your calendar, medical records, and even old texts and social media posts to remember and note when the concerning symptoms first started to appear. Document if symptoms started at a certain age, or after any other medical issues, treatments, or even vaccinations. Also, write down if your child has had any delays, or challenges with growth, development, speech, hearing etc. that are not typical for most children.
3. Take Photos
If you or your child has rashes, swollen eyes, mouth ulcers, swollen joints, or any other symptom you can get a photo of, then do take pictures to include in your log. You need to show these to any doctor you see for these symptoms. Because these symptoms may disappear as quickly as they appear, they may be gone by the time you get to the doctor’s office.
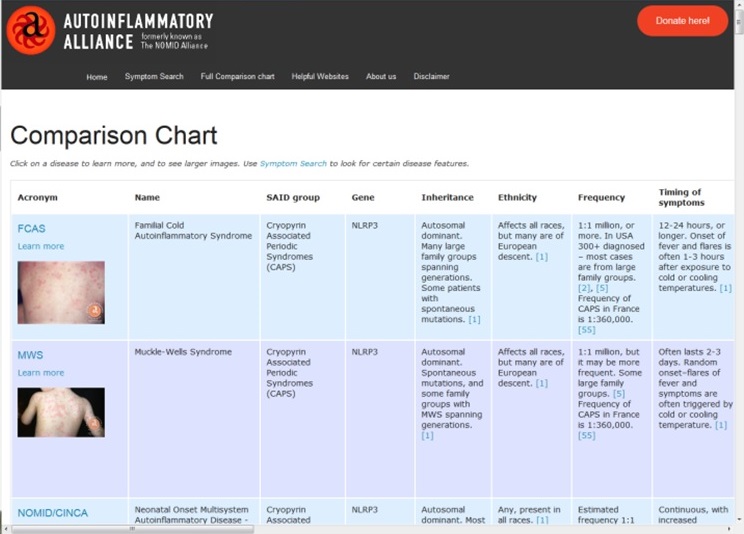 4. Print and Share Information from the Autoinflammatory Database (Share This Link) with Your Doctors
4. Print and Share Information from the Autoinflammatory Database (Share This Link) with Your Doctors
This is the Comparison Chart of Systemic Autoinflammatory Diseases. It covers most of the known periodic fever syndromes that include fever as a primary symptom. Print out pages of syndromes that stand out to you and highlight symptoms you are seeing in your child or experiencing yourself to discuss with the doctor. This can help lead you in the right direction for further testing and referrals to specialists. Click here for more information on using the periodic fever comparison chart.
To get to the bottom of recurrent fevers, you will need several blood tests. Photo by alexraths/Bigstockphoto.com
5. Discuss Blood and Other Tests You Need with Your Doctor
There are some basic tests that you should discuss with your doctor. These will help rule in or out the fever syndromes as a possible diagnosis. They will also tell you more about what is going on internally with the fevers. Additional tests may be needed for specific conditions, but listed below is a general summary of the most commonly ordered tests for periodic fever syndromes.
 This list does not cover all the tests that you may need, but are the basic tests to start with:
This list does not cover all the tests that you may need, but are the basic tests to start with:
C-reactive Protein (CRP) and Erythrocyte Sedimentation Rate (ESR)
These are inflammatory markers, and are also known as “acute-phase reactants”. They are indicators of systemic inflammation inside the body. In some fever syndromes these labs are high all the time, and can go higher during flares. While in some autoinflammatory diseases, these labs often return to normal when not in a flare. In some conditions, such as Behçet’s, the CRP and ESR may rarely, or almost never be elevated.
Complete Blood Count (CBC), with a White Blood Count (WBC) and Differential
The WBC is often high during a periodic fever syndrome flare and may or may not return to normal when the flare is over. Because a high WBC is normally associated with infections, this leads to an assumption that “it’s just a virus” or unnecessary use of antibiotics in patients with autoinflammatory diseases. It is essential to have the WBC test with the differential done, along with a CBC to get a good look at what was going on in the blood during, and after the flare, and in between flares too. Some autoinflammatory diseases that have chronic inflammation can lead to chronically elevated WBC, and certain findings in the differential. Some may also have anemia, and the CBC will help to identify trends and findings with the blood. Also, these tests are helpful to rule out blood disorders and other conditions of concern.
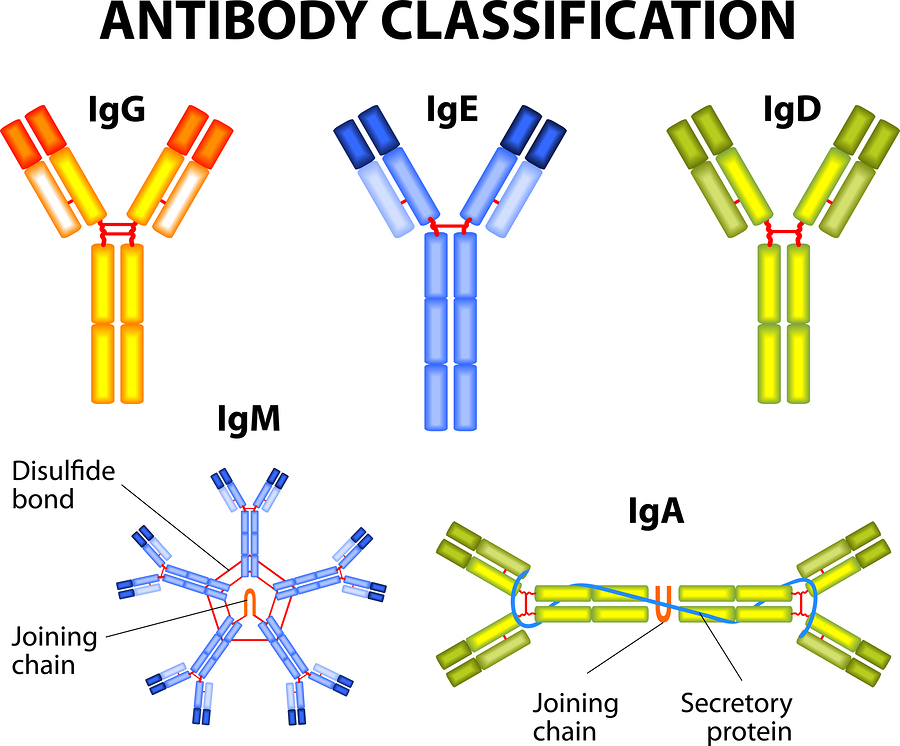
IgD, IgA, IgE, IgG, IgM
These tests relate to general immune system function, and are specific immunoglobulins. In several autoinflammatory diseases, such as PFAPA and HIDS, IgD and IgA may be high in some patients (but not all). IgE may be high in autoimmune conditions, severe allergies, and some autoinflammatory conditions. IgA, IgG and IgM may be low, but with a high IgE in patients with PLAID/FCAS3. IgA and IgM are low with APLAID. Keep in mind that doctors should not use these labs as the sole basis of a diagnosis, or to rule out a disease. These test results should be used in combination with other labs and symptoms for a diagnosis. For instance, 80% of patients with HIDS may have elevated IgD, often with IgA, but 20% do not. Young infants and children with HIDS may not show elevations in these labs until they are older. Our comparative chart has information about what Ig lab findings are often seen with each disease.
ANA
This is an antibody test. A high positive would indicate an autoimmune condition. By definition autoinflammatory condtions, aka the periodic fever syndromes, in general do not have high positive antibody tests as a symptom. However, one disease on the chart that is associated with a positive ANA is PLAID. There is also the possibility that some individuals may have both an autoimmune and autoinflammatory condition.
Fecal Calprotectin
Many autoinflammatory diseases do cause gastrointestinal symptoms including vomiting, constipation, and diarrhea. A fecal calprotectin test can detect inflammation inside the GI tract. Elevated fecal calprotectin isn’t specific or diagnostic to any one condition; many conditions can cause GI inflammation. However, doing a fecal calprotectin test can help determine if a GI specialist and more GI testing is needed.
Other tests
Doctors may order a urinalysis, cultures, and various tests to rule out infections, or other blood tests to fully evaluate the patient. This will vary for each individual. We have only discussed the most commonly ordered tests that are often ordered a few times during the initial evaluation of periodic fevers. Your doctor should decide on what is best for you or your child.
6. Repeat the Blood Tests
These tests should be repeated several times to see if there is a pattern. They should be done both during flares and when not in flares to monitor changes. Some doctors will want these tests done at the start of a flare or fever and symptoms, then repeated–sometimes weekly, or even 2-3 times a week for several weeks to get a good picture of what is happening internally. They need to see what happens with the labs during the episodes of fever and symptoms, and compare them to times when the child is not showing these symptoms, or has less symptoms. Your doctor can set up a plan for lab testing and follow up.
7. Genetic Testing
Once a periodic fever/autoinflammatory syndrome is suspected based on symptoms and initial testing, a next step is genetic testing as these syndromes are largely genetic.
Click here for more information on the genetic testing for periodic fever syndromes.
Preparing for Your Appointment
When preparing for your appointment, in addition to your symptom log, review of the history of the symptoms, and photos, also bring the link to Comparison Chart of Systemic Autoinflammatory Diseases and print out any of the disease pages that have symptoms that stand out to you with you to your doctor. Before your appointment, you should take time to highlight or circle symptoms on the chart you are seeing or experiencing. Also, do bring any literature you have read with your highlights and notes that you think fits the symptoms. And make copies of all your notes so you can keep one and give one to your doctor.
Don’t Be Afraid to Be an Advocate for Your Health
Yes, periodic fever syndrome are rare, with some only affecting a handful of patients around the world. However, they are most likely under-diagnosed, due to lack of knowledge of these diseases and because symptoms can be easily missed or misdiagnosed.
If you, or you have a son or daughter who keeps getting fevers, and you feel the symptoms of periodic fever syndromes fit you or your child, don’t be afraid to say so, and push for the testing necessary to check for these diseases. Even if you start out down the wrong path at first, bringing these concerns and symptoms to your doctor and pursuing further testing and referrals to specialists can lead you to the right diagnosis and treatment in the end.
Learn more about how autoinflammatory conditions are diagnosed here.
Read this to learn how patients can improve their health outcomes by self advocating.
The Autoinflammatory Alliance is a 501(c)(3) non-profit organization dedicated to helping those with autoinflammatory diseases.
Donate now to help with awareness, education, and research for these rare diseases.